Robotic da Vinci Sacrocolpopexy for Uterine or Vaginal Vault Prolapse
120,000+ cases of uterine and vaginal vault prolapse are surgically treated each year in the U.S. Prolapse (or falling) of any pelvic floor organ (vagina, uterus, bladder or rectum) occurs when the connective tissues or muscles within the body cavity are weak and unable to hold the pelvis in its natural orientation.
The weakening of connective tissues accelerates with age, after child birth, with weight gain and strenuous physical labor. Women experiencing pelvic organ prolapse typically have problems with urinary incontinence, vaginal ulceration, sexual dysfunction and/or having a bowel movement.
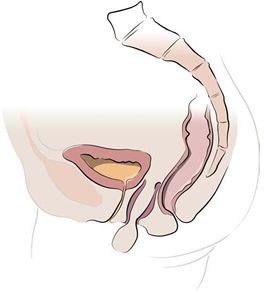
Figure 1 shows the vaginal apex (top) falling out of the vaginal opening. The view is from the side like a banana in a banana split. The bladder is in front, the vagina is falling out in the middle and the rectum is in the rear. The backbone is seen in the far right.
Treatment withh da Vinci® Sacrocolpopexy
Dr. Owens recommends sacrocolpopexy, you may be a candidate for a new surgical procedure called da Vinci Sacrocolpopexy. This procedure uses a state-of-the-art surgical system designed to help your surgeon perform a minimally invasive surgery through small incisions.
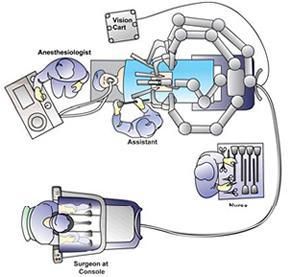
Operating Room Configuration
The robot consists of a main unit with four arms (a camera and three operating arms), and a surgeon’s console. The robot arms articulate like the human wrist and are controlled by the surgeon at the console. With 3-D optics, the surgeon is virtually inside the patient while the OR crew watches on video monitors in the room. There is a surgical assistant to pass and retrieve items from the surgical field, a scrub nurse to pass instruments, and anesthesia to monitor you during the case.
Sacrocolpopexy is a procedure to surgically correct vaginal vault prolapse where mesh is used to hold the vagina in the correct anatomical position. The term literally means lift the vagina to the pelvic bone (sacro-the portion of the back bone in the pelvis, colpos- vagina, pex-to suspend or lift up). This procedure can also be performed along with a hysterectomy to treat uterine prolapse to provide long-term support of the vagina. Long-term cure rates are about 90% as this procedure provides complete support to the vagina, especially to the top/front of the vagina that is the area most likely to prolapse. For more information click here.
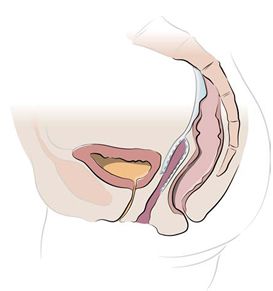
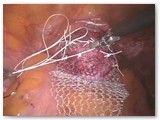
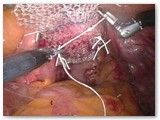
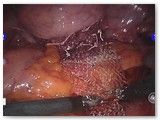
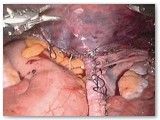
Figure 2 shows the completed sacrocolpopexy. The mesh supports the anterior apex of the vagina (weakest part of the vaginal support), as well as the posterior (back) vagina. The mesh essentially places the vagina on a leash such that it can only fall as far as the tether allows. The bladder sits on the anterior (front) mesh while the rectum gets support from the posterior (back) mesh.
For most women, da Vinci Sacrocolpopexy offers numerous potential benefits over a traditional open approach:
- Significantly less pain
- Less blood loss and need for transfusions
- Less risk of infection
- Less scarring
- Shorter hospital stay
- Shorter recovery time
- Quicker return to normal activities
As with any surgery, these benefits cannot be guaranteed, as surgery is patient- and procedure- specific.
Sacrocolpopexy has traditionally been performed as an open surgery. A 6-12 inch horizontal incision is made in the lower abdomen in order to manually access the inter-abdominal organs, including the uterus. Robotic surgery is carried out through five small incisions and the robot learns where it is in space so that the abdominal wall is not tugged on during the case. This allows for much less soreness after surgery. Most ladies in the practice go home the next day after an overnight stay in the hospital.
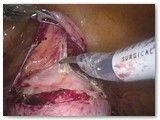
Surgery Details
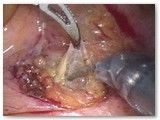
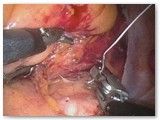
After placing the instruments into the abdomen, a form is placed into the vagina to help identify organs and aid with dissection. In this case, the patient has already had a hysterectomy some time in the past and the vaginal cuff is seen. The first step is to separate the bladder from the vagina.
Prior to viewing the surgery images below you must agree to the terms and conditions and abide by the laws of your country.
Warning:
Images in this section are of a graphic nature and include surgery and actual surgery photos. If you are under 18 years old (or 21 in some countries or regions) and/or if it is illegal in your community to view these photos, do not continue. Continuing further means that you accept full responsibility for your actions, and release Advanced Pelvic Surgery from any and all liability.